Ehsan Y. Moghadam is a PhD candidate in Mechanical Engineering. Ehsan received his MSc degree in Aerospace Engineering from Ferdowsi University of Mashhad, Iran; his research was focused on numerical analysis of heat transfer and fluid flow in microfluidics. He is currently developing micro-devices to recreate the microenvironment of neurodegenerative disease conditions. These micro-devices are utilized as alternative platforms to study the cells’ activities in a more precise, controllable, and inexpensive method. His interest is microfluidics, Micro-Electro-Mechanical Systems (MEMS), fluid mechanics, and heat transfer.
Blog post
Modeling human organs on microfluidic devices
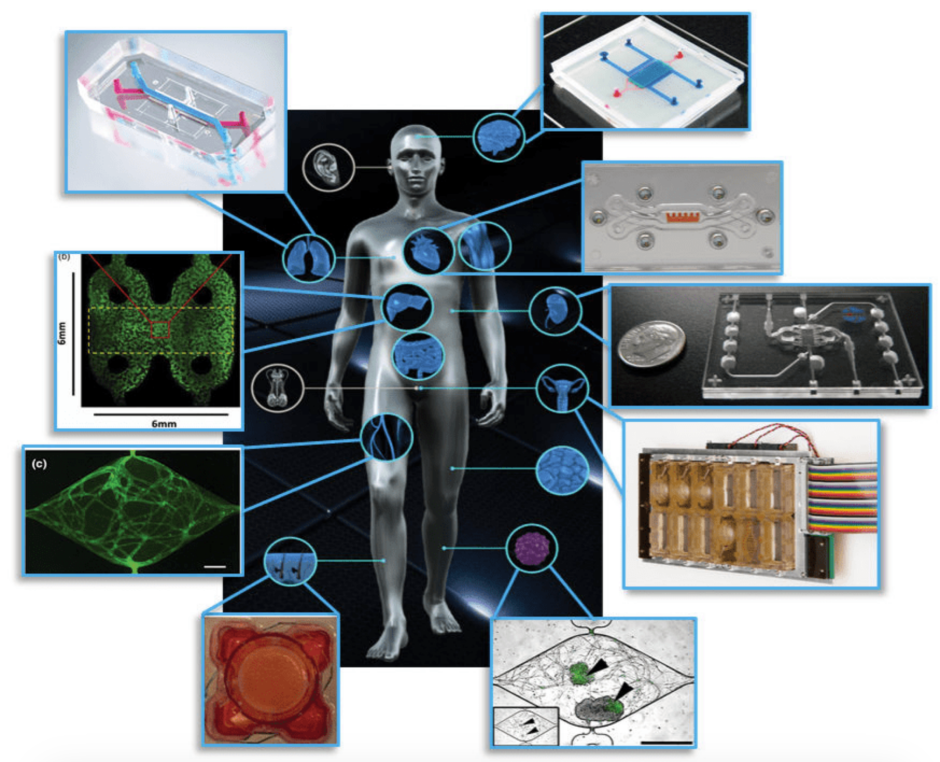 Organ-on-a-chip platforms for different organs of the body have been developed. Clockwise from top right: blood-brain barrier, cardiac muscle, kidney proximal tubule, female reproductive tract, vascularized tumor, skin epidermis, vasculature, liver, and lung-on-a-chip (L. A. Low et al., 2017)
Organ-on-a-chip platforms for different organs of the body have been developed. Clockwise from top right: blood-brain barrier, cardiac muscle, kidney proximal tubule, female reproductive tract, vascularized tumor, skin epidermis, vasculature, liver, and lung-on-a-chip (L. A. Low et al., 2017)
It is no secret that scientific research is costly. For instance, before getting an approved drug on the market, pharmaceutical companies incur costs that can easily reach $2.5 billion. Again, failures during the clinical trials can mean the drug never even makes it to the market.
To study drug mechanisms and their impact on the human body, two models are conventionally used: two-dimensional (2D) models such as standard cell culture in Petri dishes and animal models. 2D models are inexpensive, available in the bio-laboratories, and easy-to-use. However, our organs are structured in three dimensions (3D), and 2D models fail to simulate cell-cell interactions accurately. This is when it becomes essential to use animal models.
Animal models have played a crucial role in predicting pharmaceutical analysis and drug development. The drug's effects have been evaluated by testing on animal models such as mice and rabbits. But animal testing is expensive and due to the ethical issues, has been limited, and this prohibition might be extended in the future. Also, there are different species between human and animal cells and organs, which made animal models under scrutiny. For example, some anticancer drugs have different in drug uptake efficacies in animal and human cells. Also, it was found that mice could not mimic human inflammatory diseases accurately. To overcome the models' drawbacks and increase the successful human clinical trials, organ-on-a-chip models relying on microfluidics technology have been proposed.
Organ-on-a-chip
An Organ-on-a-chip is a tiny device that mimics the human body environment outside the living organism. The micro-scale-dimensions device consists of microchambers that are connected to microchannels. The cells are injected into the device’s chambers where, by providing them nutrients and same the body temperature in the sterilized condition, they grown and organize themselves in the device in a manner that emulates their natural environment. Also, the channels connected to the chambers deliver bacteria, virus, and drug to the cells and wash the cells and waste. The micro-devices are typically fabricated with a transparent, biocompatible polymer. It allows real-time imaging and monitoring of cellular responses in the device. In addition, due to micro-scale-dimensions of the micro-devices, only minimal volumes of samples and reagents are required in the experiments, which makes this method cheaper than the conventional approaches.
The simplest Organs-on-a-chip design contains a single perfused micro-chamber with two channels as the inlet and outlet, and one type of cell is grown to show the function of a type of tissue. In advanced Organs-on-a-chip, multi-layers of cells are grown to model interfaces between different tissues. The chips containing organs and tissue types can be connected. It allows for the study of drug efficacy and toxicity on different organs at the same time. Some organs-on-a-chip have been developed successfully to emulate organs such as the liver, heart, lung, intestine, kidney, brain, eye and bones-.
These micro-platforms can also manipulate the forces imposed on the cells in our body. For example, some of our body cells are always exposed to the blood flow, which creates pressure and impart stress on the cells. These can be recreated in the micro-device by adjusting the flow between the device's inlet and outlet.
Outlook
Although many advances have been achieved to mimic organ-level functions on-a-chip, the technology is still in infancy. Due to the complexities of organ functions and regular requirements, organ-on-a-chip needs more research before it can be substituted for 2D and animal models as common approaches in pharmacological studies and new drug development. Currently, the cost of manufacturing and experiments for organ-on-a-chip is still expensive, which limits research in this field. Therefore, there is an effort toward reducing cost by improving the material and methods used in the experiments. Also, to make this technology more practical and further the drug discovery process, more collaboration between medical, pharmaceutical, biological, and engineering sciences is required. The final goal of organ-on-a-chip technology is to integrate many organs into a single micro-device to make a multi-organ-on-a-chip as "Human-on-a-chip".
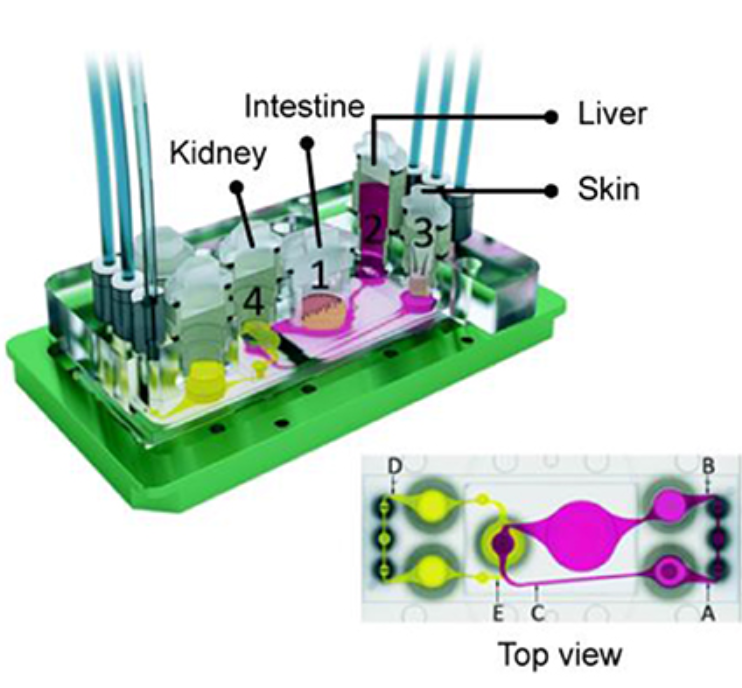 Four organ-on-a-chip, including kidney, Intestine, liver, and skin were integrated on one chip (Maschmeyer et al., 2015)
Four organ-on-a-chip, including kidney, Intestine, liver, and skin were integrated on one chip (Maschmeyer et al., 2015)
About the author


