Concurrent with their regular duties, Carnevale and his colleagues were tasked with making difficult decisions around resource allocation, such as who would benefit from the limited supply of ventilators, who would be placed on life support, and even whom to admit to the hospital.
“The hardest thing to see was the patients who were dying alone,” he recalls. “Visitors weren’t allowed then so many of those patients never got to say goodbye to their families. We would FaceTime family members so that they could see their loved ones, sometimes for the last time. That was difficult.
“We did our best to stay positive but the constant overhead alarms of patients going into cardiac arrest took a toll on all of us.”
Then there was the added stress of dealing with so much uncertainty.
“The scariest part of the whole situation was the unknown,” he says. “How long would this last? What are the lasting effects of this virus? Are we doing enough to protect ourselves and our patients?
“I would be lying if I said I wasn’t scared. But I had an incredible support system both from my wife and my co-residents and attending surgeons. Our department really pulled together during this time and Zoom helped us to check in with one another.”
In addition to testing his mettle and sharpening his professional skills, experiencing COVID-19 as a first-responder taught Carnevale about the importance of family; watching others lose loved ones only made him cherish his own family in Canada more, at a time when border closures kept them apart.
These days Carnevale is upbeat and notes that the hospital is “almost” back to normal, save for a few remaining safety protocols. With two years left of his residency, he plans to pursue academic medicine following his training; something he began while studying biology at Concordia.
“As an undergrad, I conducted independent research as part of my minor in Multidisciplinary Studies in Science. Faculty were instrumental in my development as a scientist; two of my closest mentors were Chris Brett in the Department of Biology and Andreas Bergdahl in the Department of Health, Kinesiology and Applied Physiology,” Carnevale says.
“The foundation that was built at Concordia has so far culminated in over 25 peer-reviewed publications, a dozen conference presentations and one patent. My experience at Concordia was invaluable.”


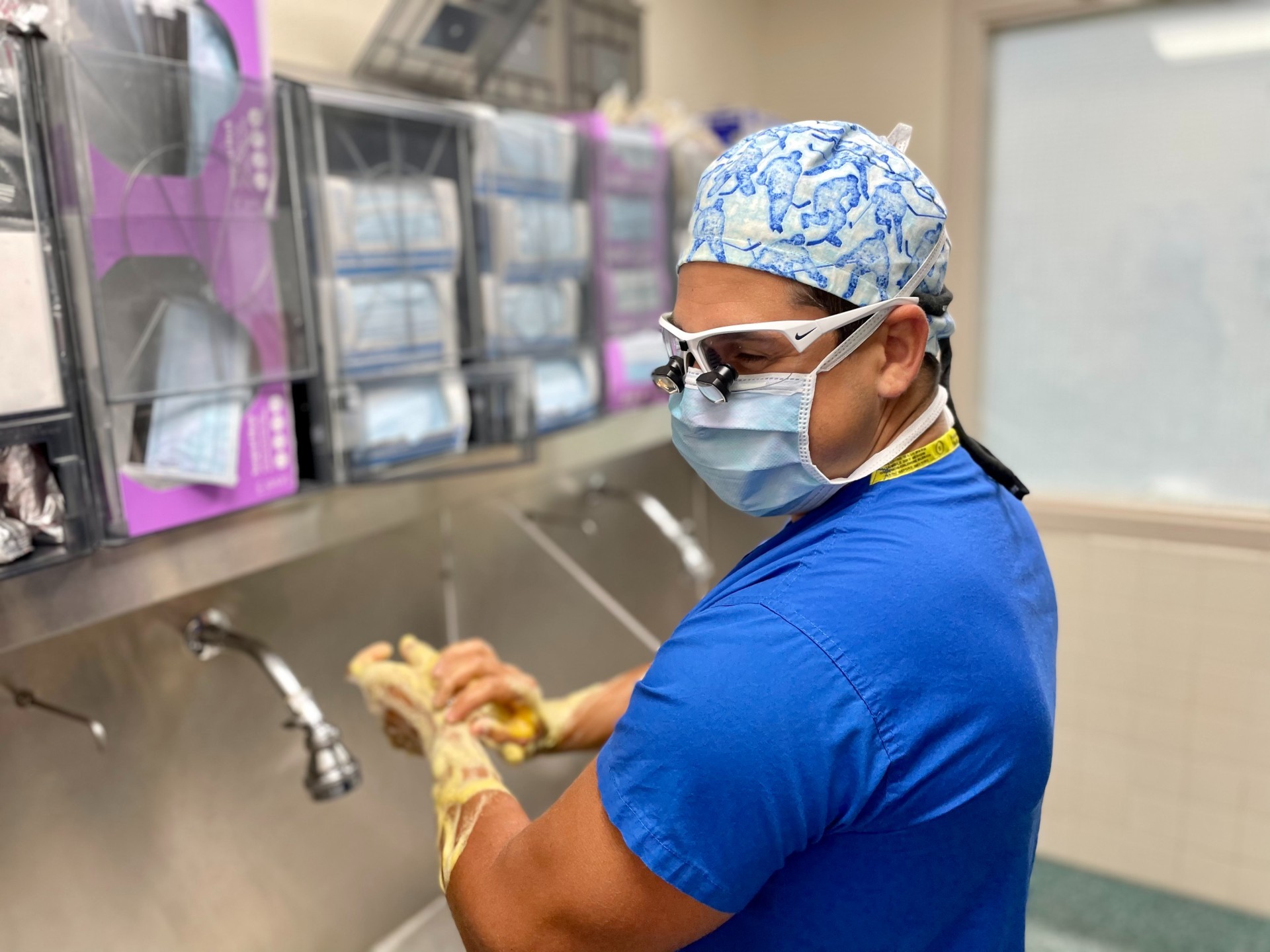 Matthew Carnevale, BSc 15, plans to pursue academic medicine after he finishes his residency.
Matthew Carnevale, BSc 15, plans to pursue academic medicine after he finishes his residency.
 “The hardest thing to see was the patients who were dying alone,” says Carnevale of his difficult work throughout the COVID-19 pandemic.
“The hardest thing to see was the patients who were dying alone,” says Carnevale of his difficult work throughout the COVID-19 pandemic.